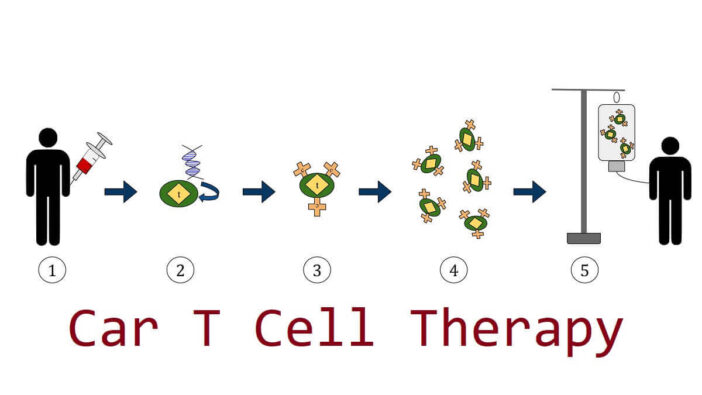
Chimeric antigen receptor T Cell therapy or Car T Cell therapy is a medical method for the treatment of cancer.
So far, medical science has not invented a screening test method to detect blood cancer early.
Blood cancer is caused by dysfunctions in the growth and behavior of cells, thus causing an excess of white blood cells that the bone marrow produces, then leads to cancer. Unfortunately, until now, there has been no screening test capable of detecting blood cancer early on.
Even so, Doctors and researchers have found the latest treatment for blood cancer. Chimeric Antigen Receptor (CAR) T Cell Therapy or CAR T Cell therapy is the latest and most modern blood cancer treatment, which provides a fairly high success rate.
What is Car T Cell Therapy?
CAR T Cell Therapy itself is believed to be the most modern blood cancer treatment method so as to provide a life expectancy for sufferers.
CAR T Cell Therapy is carried out by taking T cells in the patient and modifying them in the laboratory so that they can recognize the target of cancer in the body.
What are T cells?
T cells are white blood cells that detect and destroy abnormal cells in the human immune system.
Well, in blood cancer patients, the ability of T cells is disturbed so that they cannot detect or destroy these cancer cells.
T cells themselves are effective in treating relapsed patients with acute lymphoblastic leukemia (ALL) type blood cancer and Non-Hodgkin Lymphoma Cancer such as Diffuse Large B-Cell Lymphoma (DLBCL).
Similar to other treatments, CAR T Cell therapy also has side effects such as Immune Effector Cell-Associated Neurotoxicity Syndrome (ICANS) which affects the central nervous system.
Then the side effects of CRS or multisystemic disease that develops after treatment of CAR T cells, such as high fever and goosebumps, difficulty breathing, headache, rapid heartbeat, and so on.
CRS can appear several weeks after the process of insertion of T Cells in the body, but usually occurs within two weeks.
You Might Also Like:
Cell Wall Short Definition
Categories of Patients Who Can’t Get Car T Cell Therapy
There are several categories of patients who cannot undergo T Car cell therapy. Such as patients who have intracranial or unconscious hypertension, respiratory failure, patients with disseminated intravascular coagulation, and patients with hematosepsis or uncontrolled active infections.
How does Car T Cell Therapy Work?
In the treatment of CAR T Cells, there is a process that must be passed by the patient. It starts with a screening and taking T Cells, followed by the process of modifying T Cells.
Then do chemotherapy before the T Cells are re-inserted, the process of entering the CAR T Cells themselves, and finally the recovery and monitoring phase.
Then, the T cells are separated and transferred to the laboratory for modification. This process is carried out by inserting the Chimeric Antigen Receptor (CAR) gene into the T Cell.
The next process is to reinsert CAR T Cells into the body. In this process, the patient will be given chemotherapy to lower the number of immune cells in the body and prepare them to receive those CAR T Cells.
Once CAR T Cells begin to bind to cancer cells in the body, they will begin to increase in number and destroy cancer cells.
After completing these processes, the patient will then go through a recovery and follow-up phase. Over the next 6-8 weeks, the team of doctors will carefully monitor the patient’s condition and side effects.
Source:
- Image: Reyasingh56, CC BY-SA 4.0 https://creativecommons.org/licenses/by-sa/4.0, via Wikimedia Commons
- Video: Dana-Farber Cancer Institute



